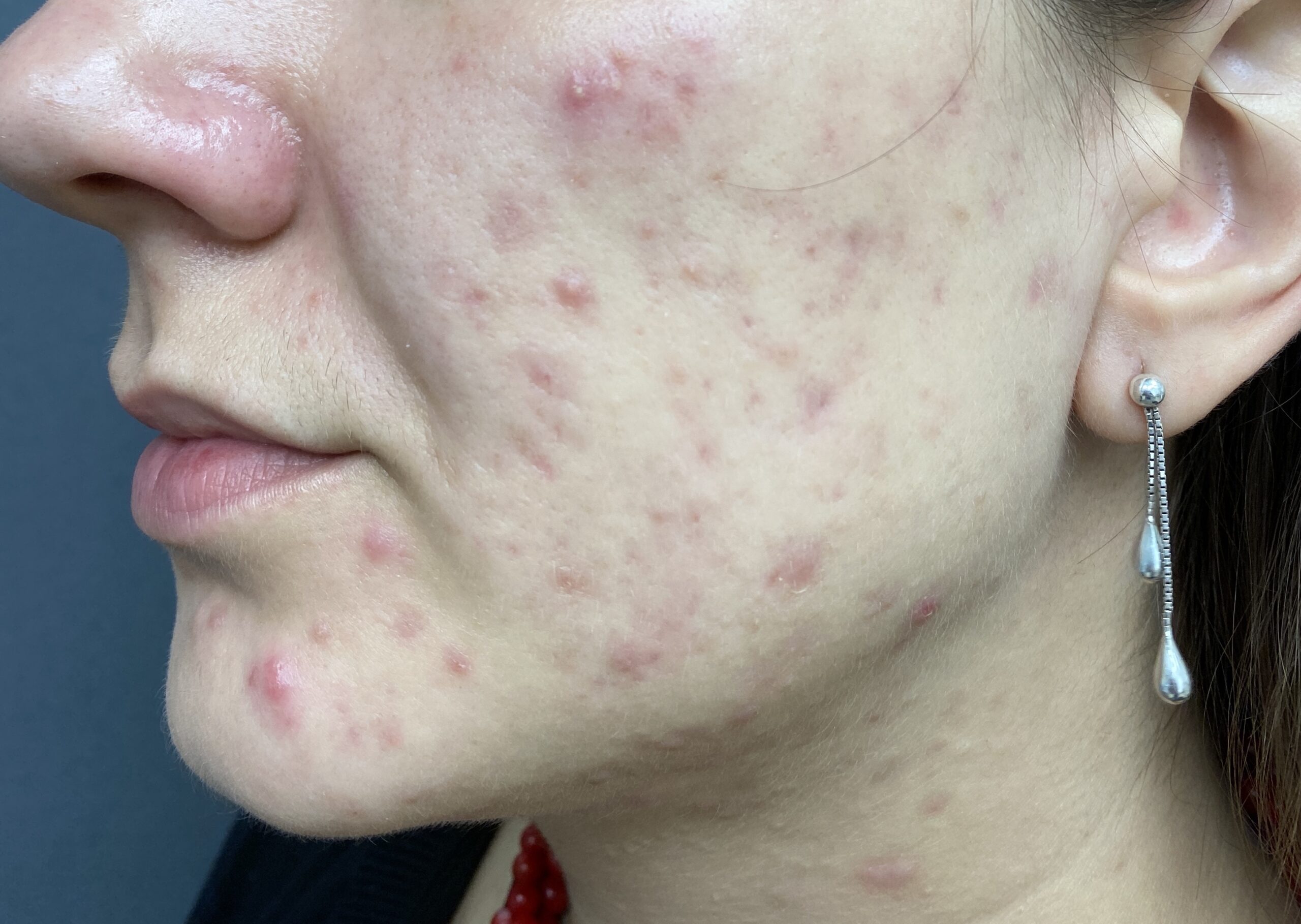
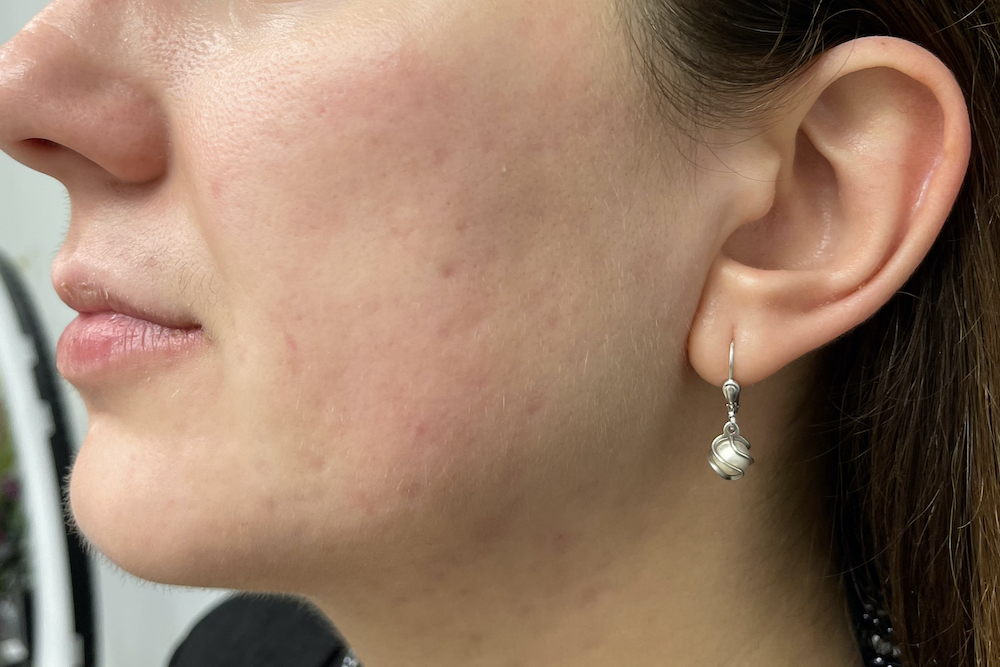
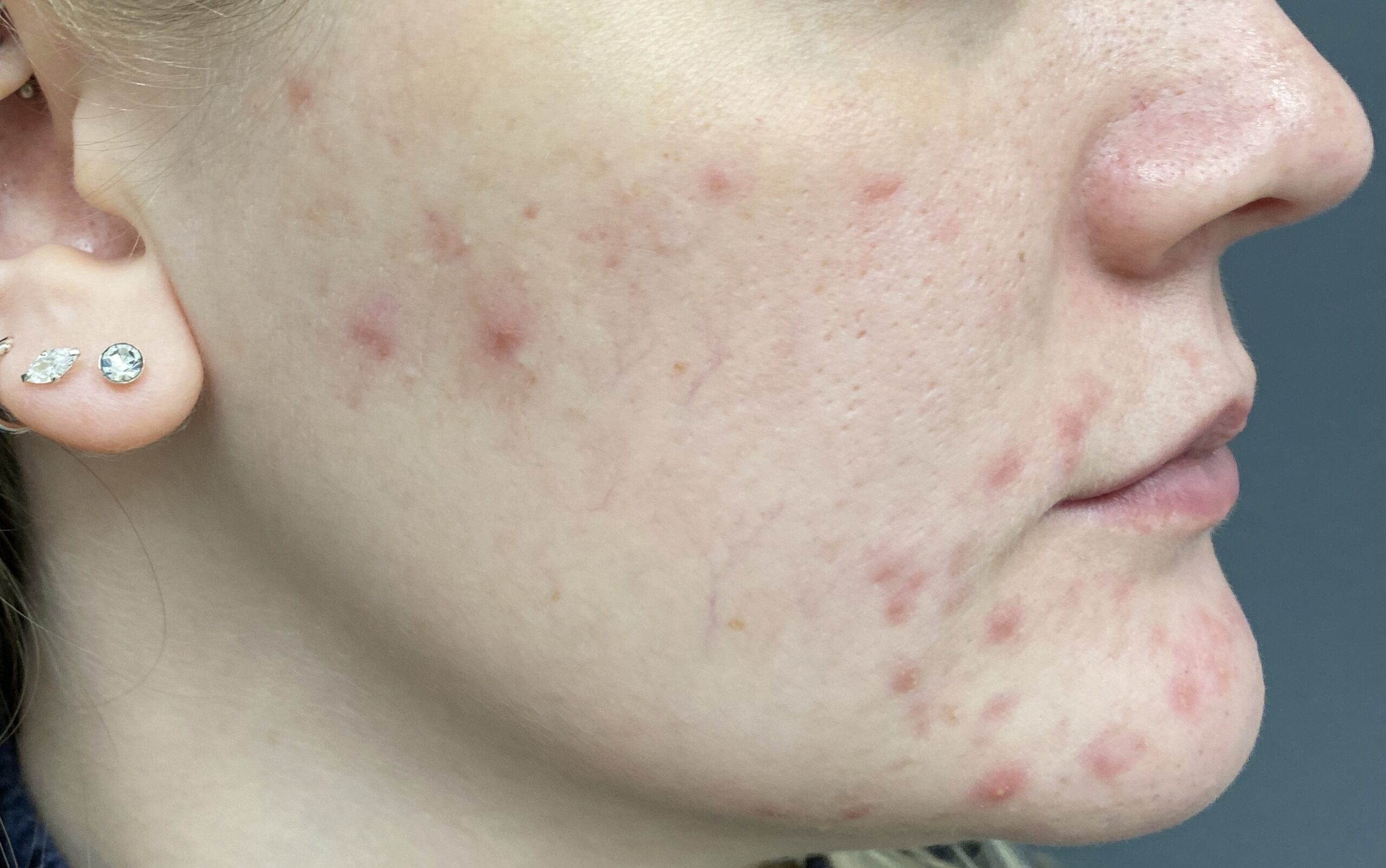
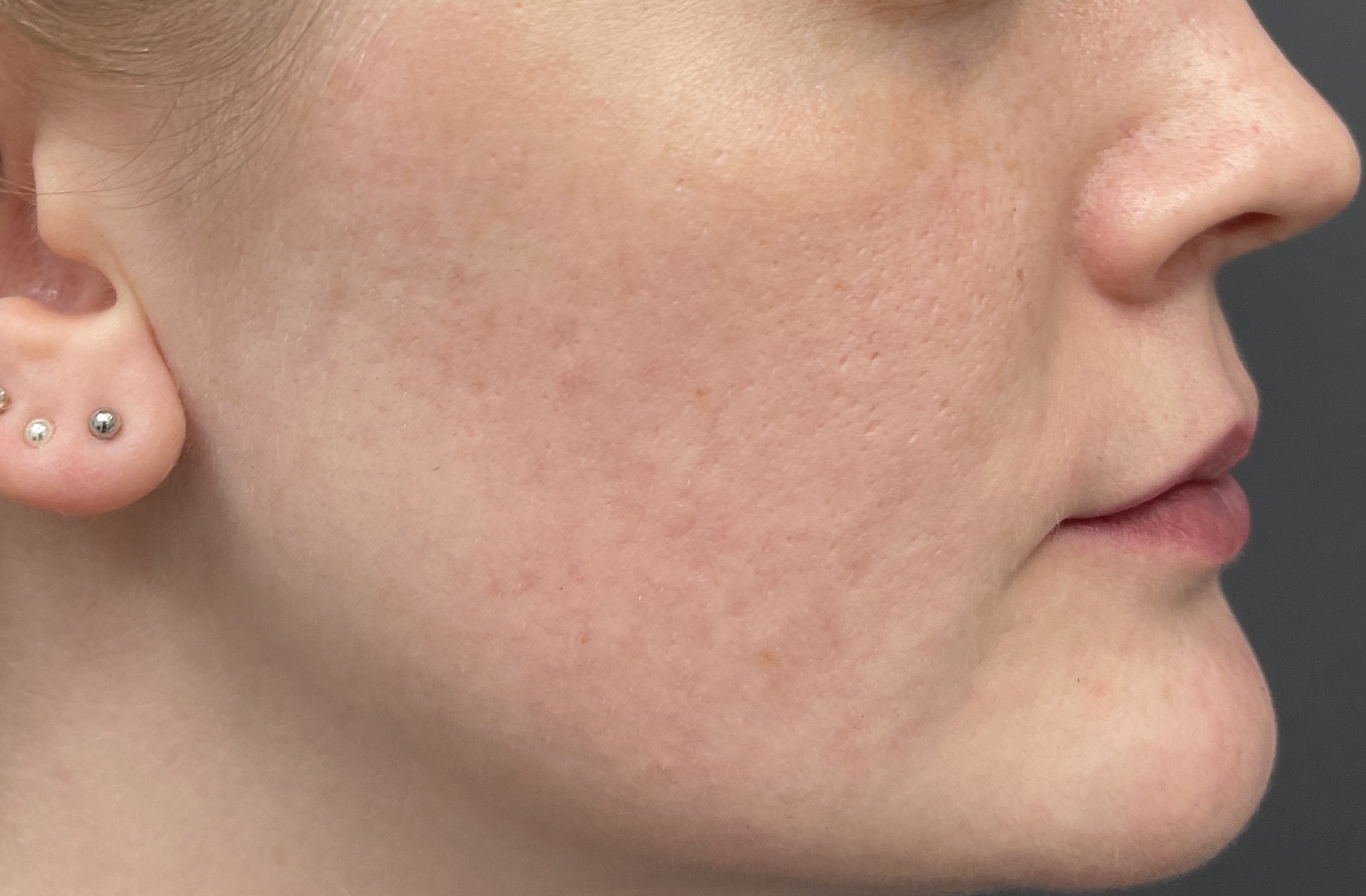
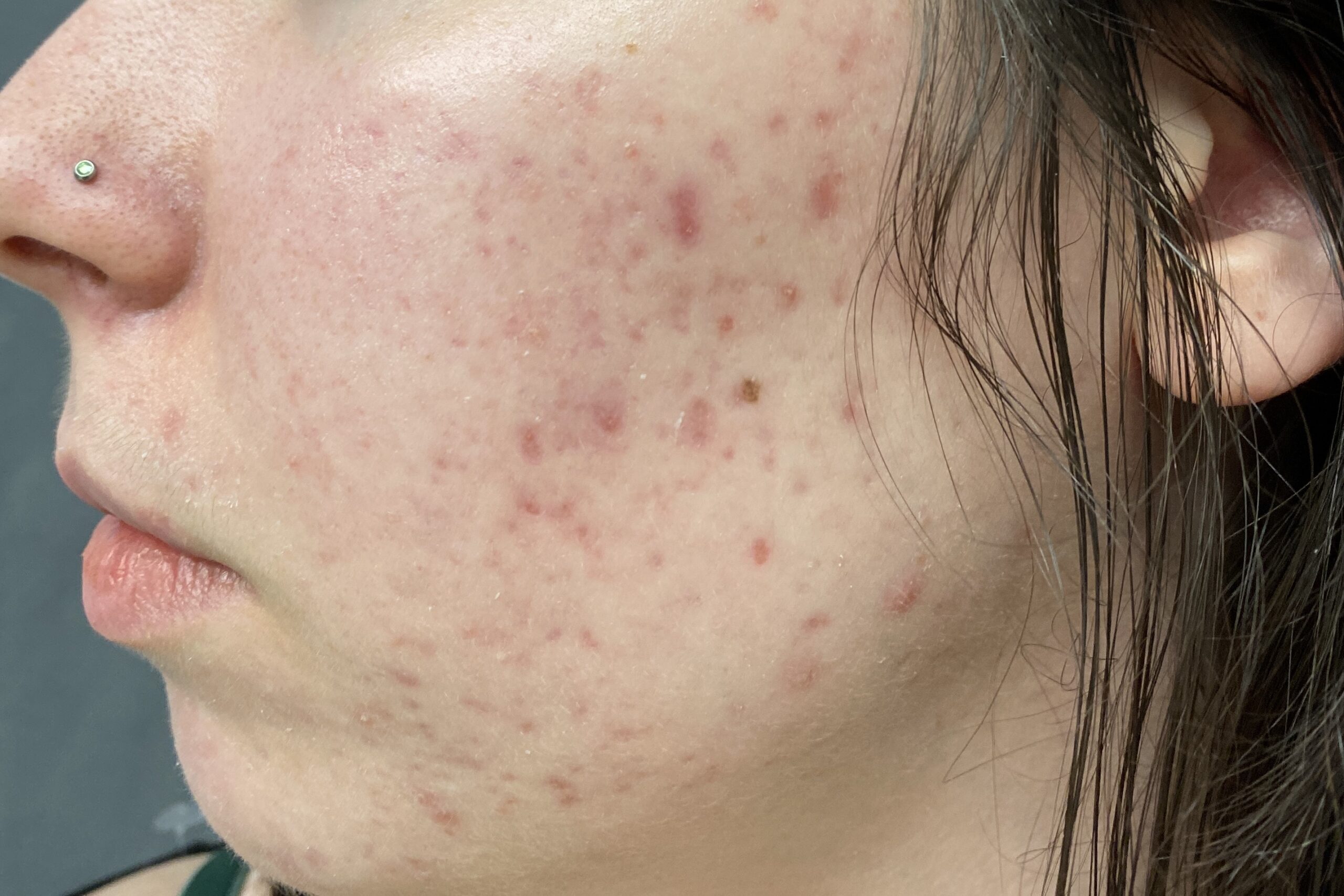
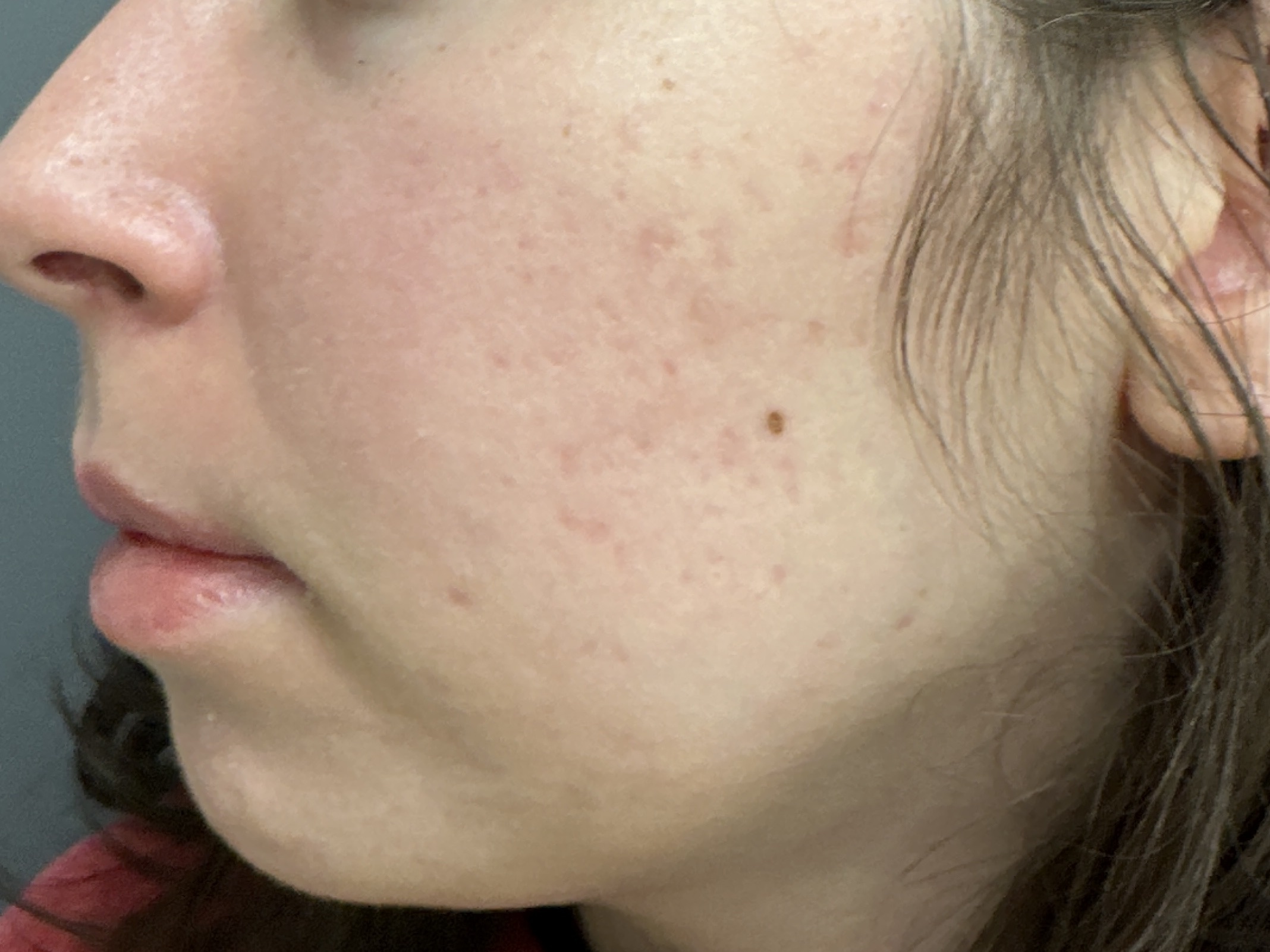
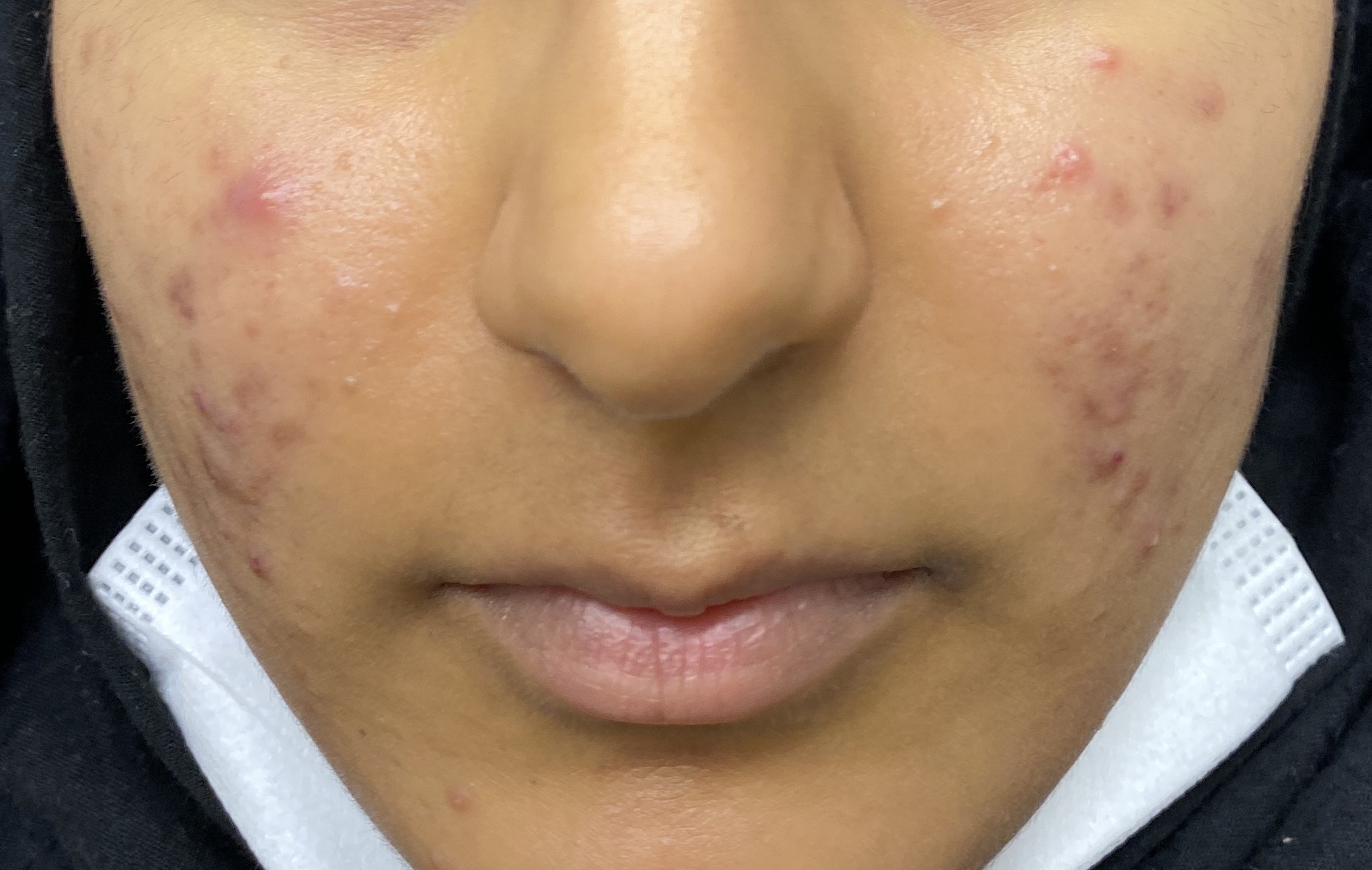
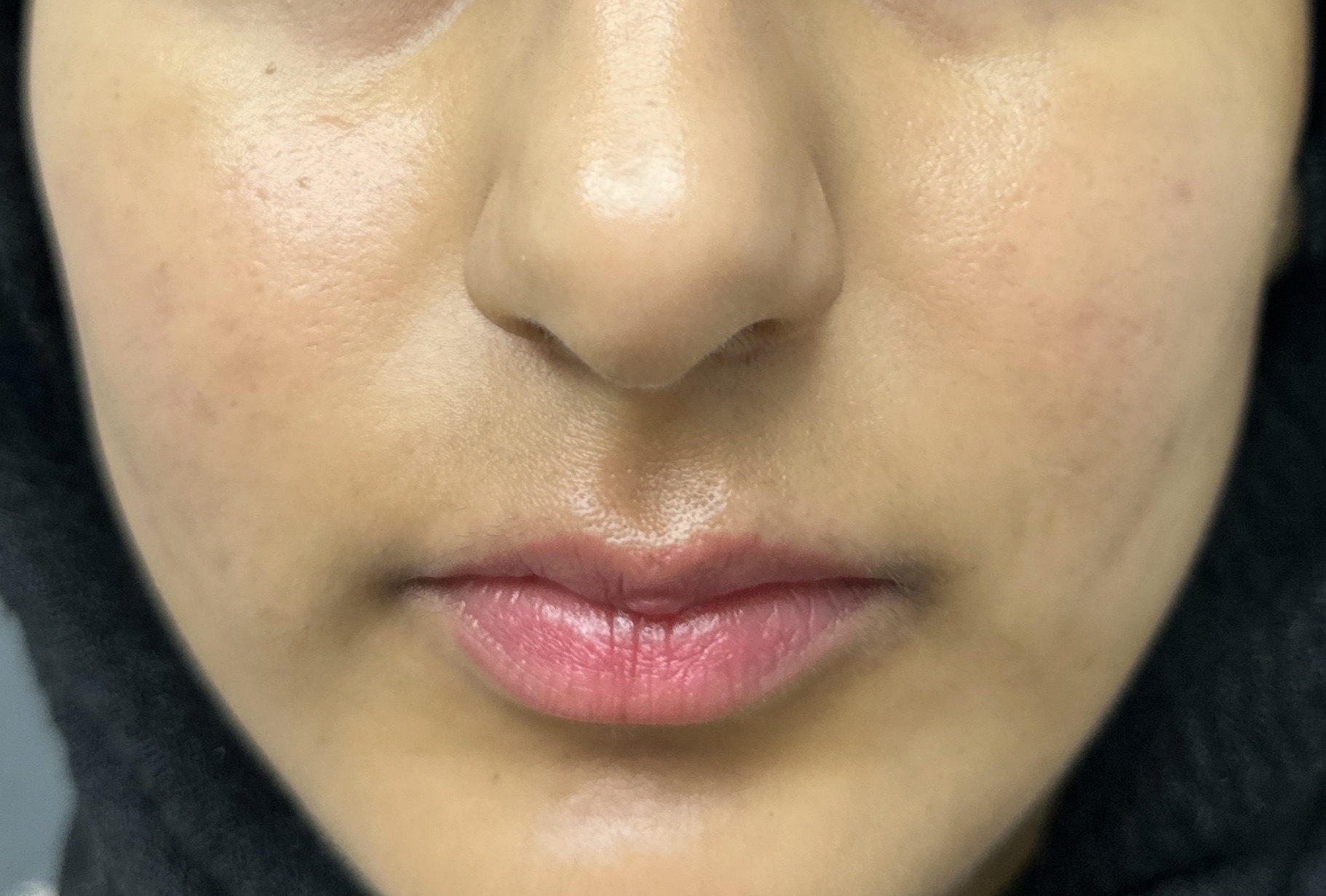
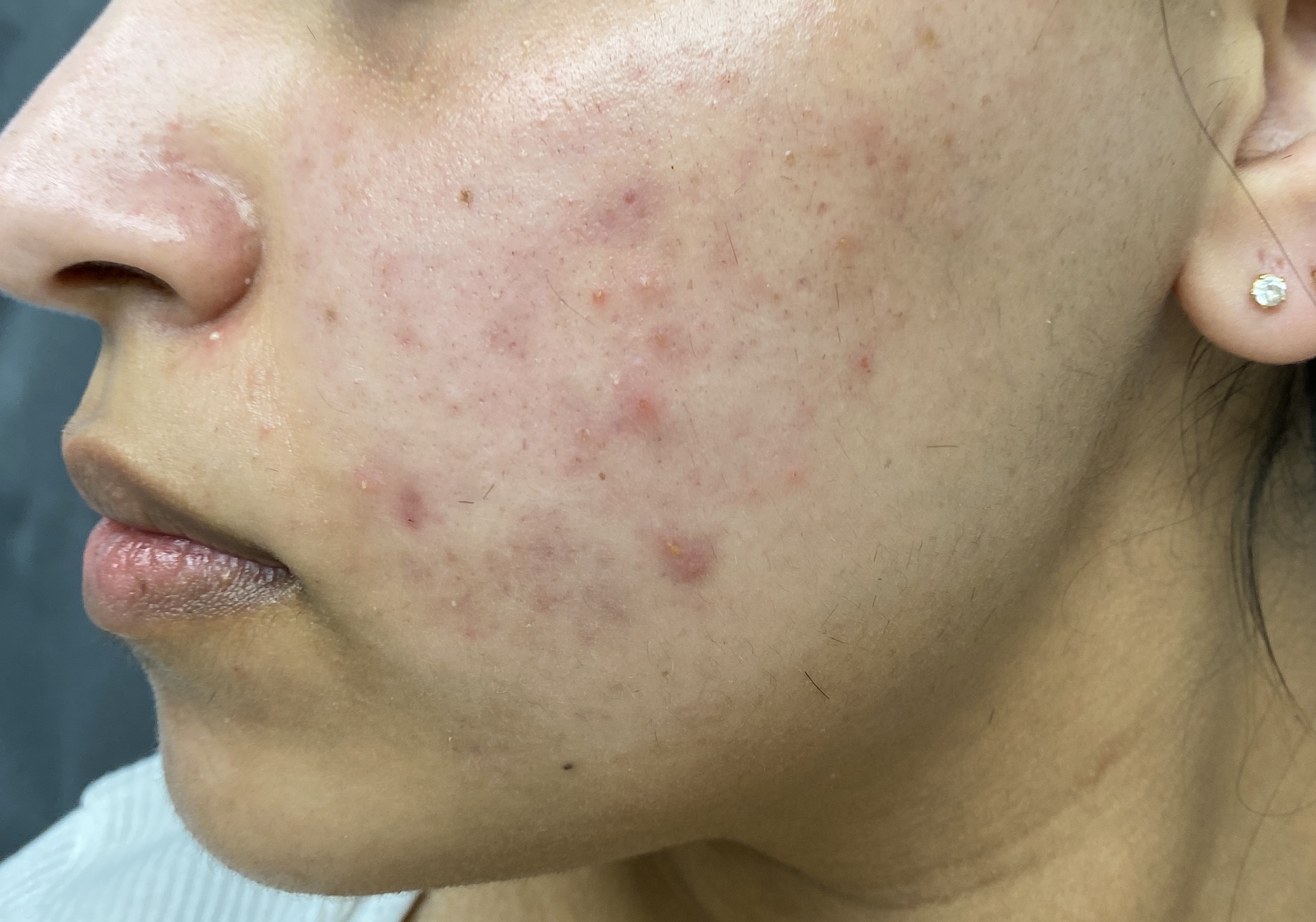
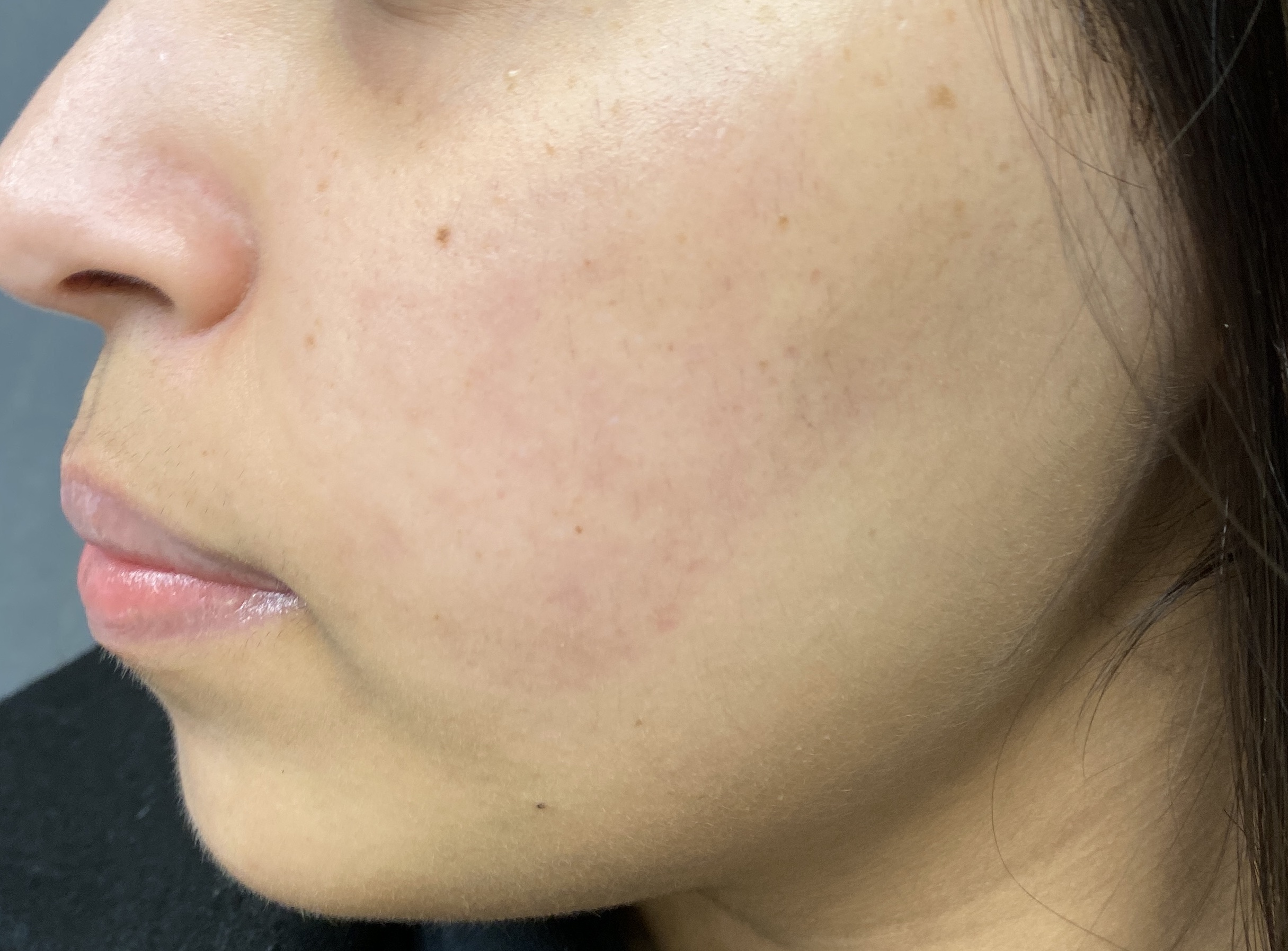
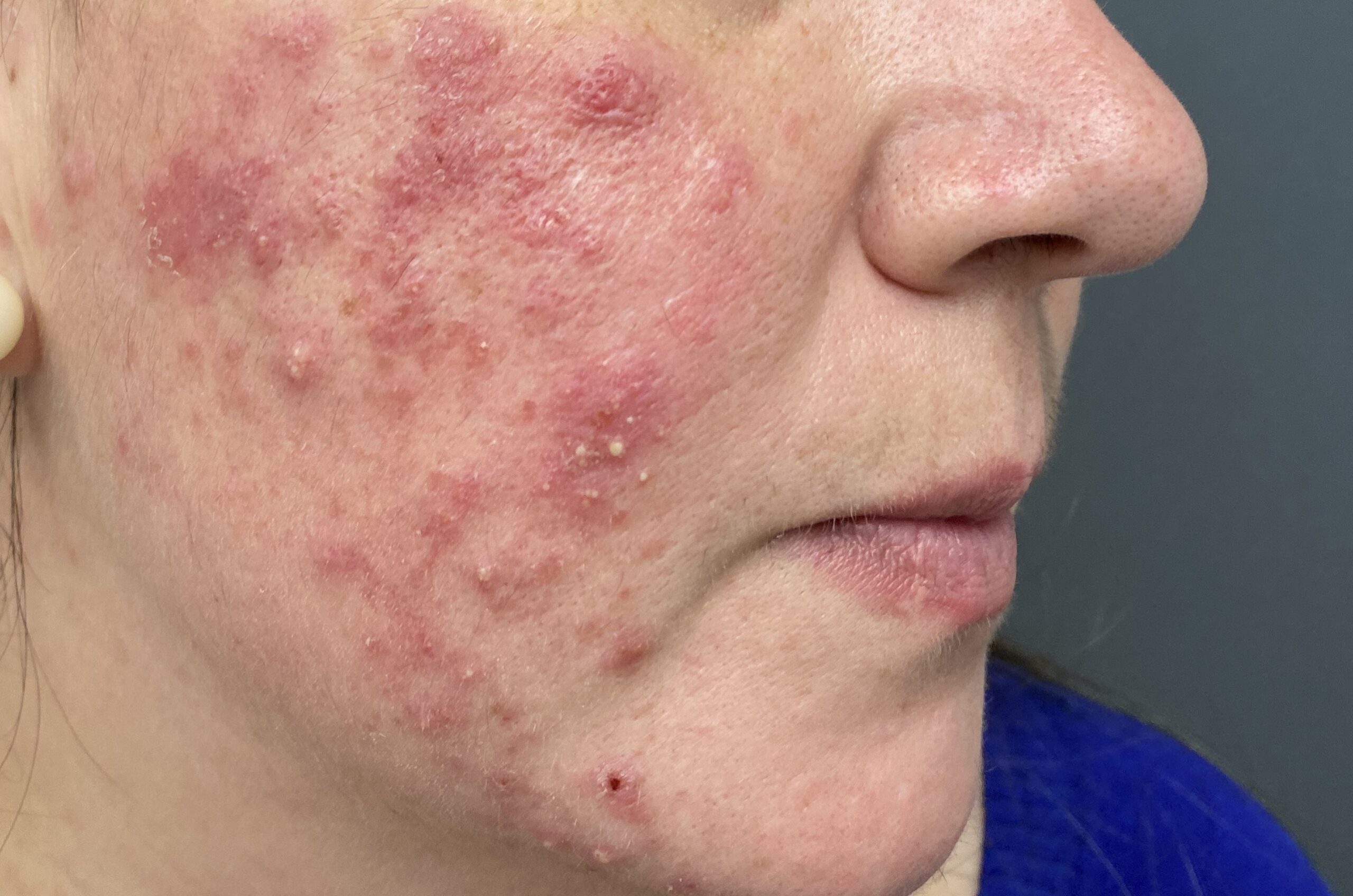
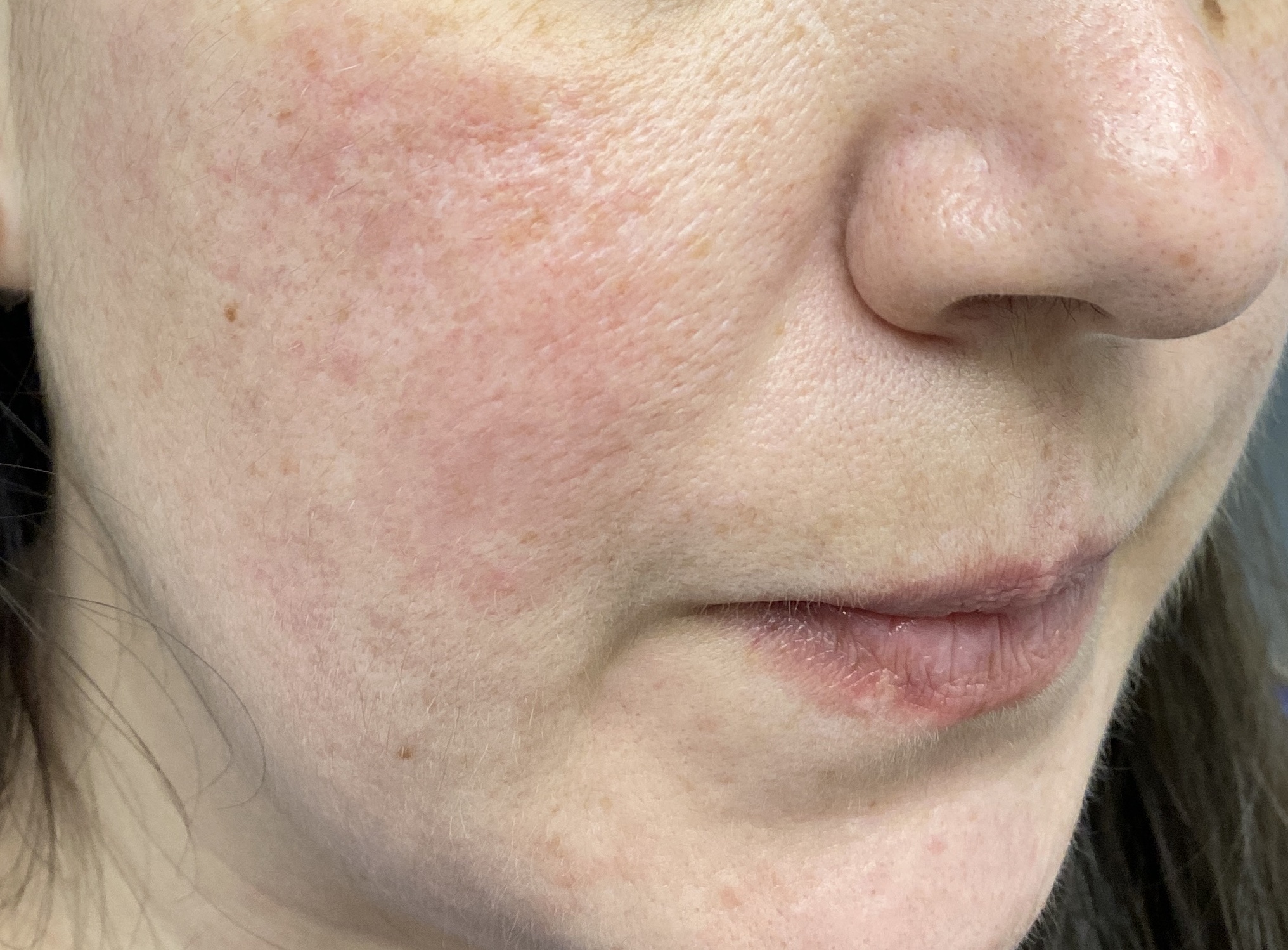
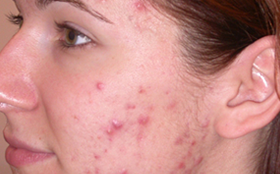
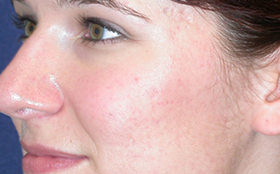
Both acne and rosacea are common inflammatory conditions of the skin that cause spots and redness on the face. However, not all face redness and spots are caused by acne or rosacea. Getting the correct diagnosis from the outset is key to determine the right treatment for you.
Dr Nicole believes in performing a detailed history and physical examination to determine the correct diagnosis, and to treat these conditions effectively at an early stage to prevent late consequences such as scarring to the face.
As a Consultant Dermatologist in Manchester, Cheshire & Lancashire, with experience in both medical and cosmetic dermatology, Dr Nicole can incorporate both her medical and cosmetic dermatology knowledge into your treatment regime. This combination of cosmetic treatments and targeted, prescription-based medical treatments can help to control your acne or rosacea and give you a lifetime of healthy skin.
Treatments that Dr Nicole offers for acne/rosacea include:
– Prescription-based topical and oral medications (oral antibiotics, oral isotretinoin, oral spironolactone)
– Lasers including Aviclear laser to treat acne, Excel V+ and Enlighten SR lasers to treat uneven skin tone due to post-inflammatory acne marks, rosacea redness/red veins/flushing and pigmentary changes
- Assessment and treatment by a Consultant Dermatologist with an interest in both medical and cosmetic dermatology
- A systematic approach to determine the cause and triggers to your problem to prevent flare-ups of your acne/rosacea
- Individualised treatment plans with recommended skincare regime to treat the disease and its causes
- Effective preventative programme to combat disease at an early stage
- Combined treatment approaches to tackle both the medical and cosmetic aspects of acne/rosacea
- No GP referral required